Vagus Nerve: The Silent Controller of Your Mental Health
Vagus nerve dysfunction disrupts your body's natural stress recovery and emotional regulation systems, contributing to persistent anxiety, depression, and trauma responses, but evidence-based therapeutic approaches including polyvagal therapy and nervous system regulation techniques effectively restore healthy vagal tone and mental wellness.
What if the key to understanding your anxiety, depression, and stress recovery isn't in your brain, but in a nerve you've probably never heard of? The vagus nerve controls more of your mental health than you might imagine.
In this Article
What is the vagus nerve? Anatomy made simple
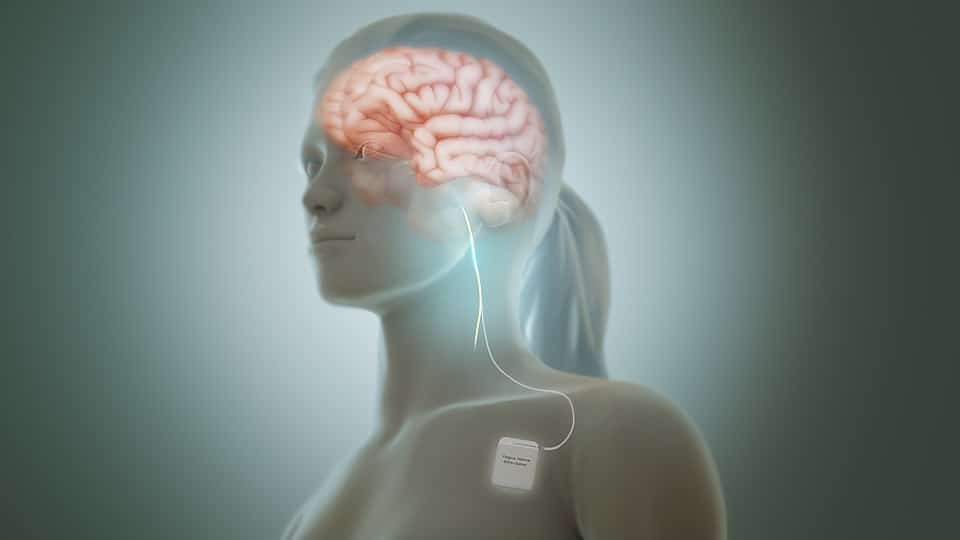
Your body has a hidden communication superhighway running from your brain to your gut, and most people have never heard of it. The vagus nerve is the longest cranial nerve in your body, stretching from your brainstem all the way down through your neck, chest, and into your abdomen. Its name comes from the Latin word for “wandering,” which makes perfect sense once you understand how far this nerve travels and how many organs it touches along the way.
Picture two long, thin cords of nerve fibers, one on each side of your body. These branches travel alongside major blood vessels in your neck, tucked behind your carotid artery. From there, they branch out like tree roots, sending smaller fibers to your heart, lungs, stomach, intestines, and other vital organs. The vagus nerve’s location in the neck is particularly significant because this is where many therapeutic techniques target the nerve.
What makes the vagus nerve truly remarkable is its role as your body’s main parasympathetic controller. It manages your “rest and digest” functions: slowing your heart rate when you’re calm, triggering digestive processes after meals, regulating immune responses, and even influencing your mood. When your vagus nerve is working well, your body can shift smoothly between states of alertness and relaxation.
Here’s something that surprises most people: about 80% of vagal nerve fibers are afferent, meaning they carry information to the brain rather than from it. Your vagus nerve is constantly sending updates about what’s happening in your body, from your gut bacteria activity to your heart rhythm. Your brain isn’t just telling your body what to do. Your body is also telling your brain how it feels, and the vagus nerve is the primary messenger.
How the vagus nerve affects mental health
Your brain doesn’t operate in isolation. It’s constantly receiving signals from the rest of your body, and the vagus nerve serves as the primary messenger. This two-way communication system influences everything from your mood to how quickly you bounce back after a stressful day.
The vagus nerve, inflammation, and mood
One of the vagus nerve’s most critical jobs involves regulating your body’s inflammatory response. When the nerve functions well, it releases acetylcholine, a neurotransmitter that calms inflammation throughout your body. Chronic inflammation has been consistently linked to depression, which helps explain why some people with persistent low moods don’t respond to traditional treatments alone.
The vagus nerve also influences the production of key neurotransmitters in your gut, including serotonin and GABA. These chemicals play essential roles in mood regulation, sleep, and feelings of calm. When vagal function is compromised, the entire system can fall out of balance.
What is the connection between the vagus nerve and anxiety?
Your nervous system has two main modes: fight-or-flight and rest-and-digest. The vagus nerve is responsible for activating that second, calmer state. When it’s working properly, you can experience stress and then return to baseline relatively quickly. Your heart rate slows, your breathing deepens, and your body signals safety to your brain.
People with low vagal tone often struggle to make this shift. Their bodies stay stuck in a heightened state of alertness, which can manifest as persistent anxiety or even panic attacks. The vagus nerve and anxiety attacks are closely connected because poor vagal function means your body cannot send the “all clear” signal that helps you feel safe again.
Research has found that low vagal tone is associated with depression, PTSD, and difficulty recovering from stressful experiences. Vagal tone isn’t fixed, though. You can strengthen vagus nerve function through specific practices and lifestyle changes.
Understanding polyvagal theory: Your three nervous system states
If you’ve ever wondered why you can feel perfectly fine one moment and completely overwhelmed the next, polyvagal theory offers a compelling explanation. Developed by neuroscientist Dr. Stephen Porges, this framework describes three distinct states your nervous system moves between throughout the day. Each state shapes how you think, feel, and connect with others.
The vagus nerve acts as the primary regulator of these states, constantly scanning your environment for signals of safety or danger. Your nervous system makes these assessments automatically, often before your conscious mind catches up. Understanding which state you’re in can help explain why some coping strategies work beautifully on certain days and fall flat on others.
Ventral vagal: The safe and social state
This is your optimal state for mental health and wellbeing. When your ventral vagal system is active, you feel calm, present, and genuinely connected to the people around you. Your heart rate is steady, your breathing is relaxed, and your facial muscles naturally soften.
In this state, you can think clearly, solve problems creatively, and engage in meaningful conversations. You feel curious rather than threatened. Challenges seem manageable, and you have access to your full range of emotional responses. You can form and maintain healthy relationships because your nervous system signals that it’s safe to be vulnerable with others.
Sympathetic activation: Fight or flight
When your nervous system detects a threat, it shifts into sympathetic activation. Your heart pounds, muscles tense, and breathing becomes shallow and rapid. This is the anxious, agitated state most people recognize as stress.
In fight mode, you might feel irritable, defensive, or quick to anger. In flight mode, you experience the urge to escape, avoid, or withdraw from situations. Panic attacks, chronic anxiety, and persistent worry often reflect a nervous system stuck in this mobilized state. While this response evolved to protect you from immediate physical danger, it can become problematic when it activates in response to everyday stressors like work emails or social situations.
Dorsal vagal: Shutdown and freeze
When fight or flight feels impossible or ineffective, your nervous system may drop into its oldest survival response: shutdown. The dorsal vagal state brings numbness, disconnection, and a sense of collapse. You might feel foggy, exhausted, or emotionally flat.
This state often underlies symptoms of depression, dissociation, and chronic fatigue. People describe feeling frozen, stuck, or like they’re watching life from behind glass. It’s your body’s last-resort protection mechanism, designed to help you survive overwhelming situations by conserving energy and reducing awareness of pain.
Many trauma-informed approaches in therapy now focus on helping people recognize these states and build capacity to return to ventral vagal safety. Mental health symptoms often reflect which nervous system state has become your default setting. When you understand your patterns, you gain valuable insight into why certain interventions resonate with you while others miss the mark entirely.
Signs and symptoms of poor vagal tone
Your vagus nerve doesn’t come with warning lights or error messages. When it’s not functioning well, the signs show up across your entire system, often in ways that seem unrelated. You might not connect your digestive troubles to your anxiety, or your brain fog to your social discomfort. But they may all trace back to the same root: low vagal tone.
Physical signs
Poor vagal tone often shows up in your body first. You might notice persistent digestive issues like bloating, constipation, or a heavy feeling after eating. Your heart rate may run faster than normal, even at rest, or you might feel your heart pounding during minor stress. Some people experience difficulty swallowing or a sensation of tightness in the throat. Chronic inflammation can also signal vagal dysfunction, since the vagus nerve plays a key role in calming your body’s inflammatory response.
Emotional signs
When your vagus nerve isn’t working optimally, calming down after stress becomes genuinely difficult. Anxiety might feel less like worried thoughts and more like something trapped in your chest or stomach. You may swing between feeling overwhelmed and emotionally numb. That stuck quality to emotions, where they linger long after the trigger has passed, often points to vagal involvement.
Cognitive and social signs
Brain fog and difficulty concentrating are common with low vagal tone. You might feel disconnected from your surroundings, like you’re watching life through a window. Social situations can feel unusually draining or even threatening. Reading facial expressions becomes harder, and you may find yourself avoiding eye contact without knowing why. These responses happen because the vagus nerve helps regulate your sense of safety around others.
Slow recovery patterns
One of the clearest indicators of poor vagal tone is how long it takes you to bounce back. Whether it’s recovering from a cold, processing a stressful event, or returning to baseline after an argument, slow recovery suggests your nervous system struggles to shift back into rest mode. Tracking your recovery patterns can reveal a lot about your vagal health.
How to measure your vagal tone: the HRV guide
Heart rate variability (HRV) has become the gold standard for measuring vagal tone outside clinical settings. It’s accessible, trackable, and gives you real data about your nervous system’s flexibility.
HRV measures the tiny variations in time between each heartbeat. A healthy heart doesn’t beat like a metronome. Instead, it speeds up and slows down in response to your breathing, thoughts, and environment. This variability reflects how well your vagus nerve communicates with your heart.
What HRV numbers mean and how to interpret yours
Higher HRV generally indicates better vagal tone and greater stress resilience. Lower HRV often signals that your body is stuck in a more rigid stress response. The most relevant HRV metric for vagal function is called RMSSD (root mean square of successive differences), which specifically captures the parasympathetic influence on your heart rate. Here’s what typical RMSSD ranges look like:
- Ages 20-29: Women average 35-55 ms, men average 40-60 ms
- Ages 30-39: Women average 30-50 ms, men average 35-55 ms
- Ages 40-49: Women average 25-45 ms, men average 30-50 ms
- Ages 50+: Women average 20-40 ms, men average 25-45 ms
These are general benchmarks. Your personal baseline matters more than comparing yourself to population averages. Track your own trends over time rather than fixating on hitting a specific number.
Taking accurate HRV measurements
Consistency is everything when tracking HRV. Take your measurements first thing in the morning, before coffee or checking your phone. Your body is in its most neutral state after sleep, giving you the clearest picture of your baseline vagal function.
Use the same device and body position each time. Chest straps provide the most accurate readings, though finger sensors and smartwatches have improved significantly. Sit or lie down in the same position for at least one minute before recording. Several apps offer validated HRV tracking, including Elite HRV, HRV4Training, and the Oura Ring app. Many newer Apple Watches and Garmin devices also provide reliable RMSSD measurements.
Set realistic expectations for improvement. Expect 4 to 12 weeks of consistent vagal toning practices before seeing meaningful changes in your numbers. Your nervous system adapts gradually, not overnight.
Evidence-based ways to stimulate your vagus nerve
Vagal tone can genuinely be improved. The vagus nerve responds to specific activities and lifestyle choices, and with consistent practice, these techniques can help shift your baseline from chronic stress toward greater calm and resilience.
Breathing techniques for vagal activation
Your breath is the most direct way to communicate with your vagus nerve. Slow, deep breathing with extended exhales sends a clear signal to your nervous system that you’re safe. The key is making your exhale longer than your inhale, which activates the parasympathetic response.
Try breathing in for four counts, then breathing out for six to eight counts. Even five minutes of this practice can measurably increase heart rate variability. Breath work is free, portable, and available to you in any stressful moment.
Other accessible vagal activation practices
Cold exposure triggers what’s called the dive reflex. Splashing cold water on your face or ending your shower with 30 seconds of cold water activates vagal pathways almost immediately. Start small if you’re new to this, as even brief cold exposure can produce calming effects.
Humming, singing, and gargling all vibrate the vagus nerve where it passes through your throat. This is why singing in the car or humming while you cook can feel so naturally soothing. Gargling water vigorously for 30 to 60 seconds each morning is a simple way to give your vagus nerve a workout.
Social connection plays a powerful role in vagal health. Safe, supportive relationships activate the ventral vagal system, the branch associated with feeling calm and connected. Spending time with people who make you feel at ease isn’t just emotionally satisfying; it’s physiologically regulating.
Movement practices like yoga and tai chi have been shown to improve vagal tone over time. These gentle, rhythmic activities combine breath awareness with physical movement, creating ideal conditions for nervous system regulation. Mindfulness-based practices can complement these approaches by building greater awareness of your body’s stress signals.
Gut health matters too, since the vagus nerve is the primary communication pathway between your gut and brain. Eating an anti-inflammatory diet rich in fiber and fermented foods supports the beneficial bacteria that send calming signals through vagal pathways.
What are the benefits of stimulating the vagus nerve for mental health?
Regular vagus nerve stimulation can produce meaningful changes in how you feel day to day. People who practice these techniques often report feeling less reactive to stress, recovering more quickly from difficult emotions, and experiencing fewer symptoms of anxiety. Improved vagal tone also supports better sleep, more stable mood, and a greater sense of groundedness. Over time, these practices can help shift your nervous system’s default settings, making calm feel more accessible even during challenging periods.
The trauma-vagus connection: why talk therapy isn’t always enough
If you’ve ever talked through a traumatic experience, understood it logically, and still felt your body react as though the danger were happening right now, you’ve experienced something important. Trauma doesn’t just live in your memories. It lives in your nervous system.
When someone experiences trauma, the vagus nerve can become dysregulated, essentially getting stuck in survival mode. The body might remain locked in a fight-or-flight state, constantly scanning for threats that no longer exist. Or it might shift into a freeze response, leaving a person feeling numb, disconnected, or unable to engage with life fully. These aren’t character flaws or signs of weakness. They’re nervous system adaptations that once served a protective purpose.
Traditional talk therapy, while valuable, primarily engages the thinking brain. You can gain insight into why you react certain ways, develop new perspectives on past events, and build coping strategies. But if the vagus nerve itself remains dysregulated, your body may continue responding to triggers before your conscious mind even registers what’s happening. This is why some people feel frustrated after years of therapy: they understand their trauma intellectually, yet their bodies haven’t received the message that they’re safe.
This is where body-based approaches become essential. Somatic experiencing helps you gradually release trauma stored in the body by tracking physical sensations. EMDR uses bilateral stimulation to help the brain reprocess traumatic memories. Sensorimotor psychotherapy combines talk therapy with body awareness to address trauma at multiple levels simultaneously.
Polyvagal-informed therapy adds another layer by helping you understand your nervous system responses without shame. When you recognize that your reactions stem from vagal states rather than personal failings, something shifts. You stop blaming yourself for responses that were never within your conscious control.
For people with trauma-related conditions, combining cognitive approaches with somatic work often produces the most lasting results. A trauma-informed therapist can help you identify which combination of approaches fits your specific needs and nervous system patterns.
If you’re curious whether trauma-informed or somatic approaches might help, ReachLink offers a free assessment to match you with a licensed therapist who specializes in nervous system-based treatment, with no commitment required.
Vagus nerve dysfunction in specific conditions
Many chronic conditions share a common thread: disrupted communication along vagal pathways. Understanding how vagal function relates to specific health conditions can help make sense of symptoms that might otherwise seem unconnected.
Digestive disorders and the gut-brain axis
If you live with irritable bowel syndrome or other functional digestive disorders, vagus nerve dysfunction may play a significant role in your symptoms. The vagus nerve transmits signals about digestion, inflammation, and even the state of your gut microbiome. When this communication breaks down, you might experience heightened sensitivity to normal digestive processes, irregular motility, and increased gut inflammation. Stress makes everything worse because it suppresses vagal activity, which explains why digestive symptoms often flare during anxious periods.
Chronic fatigue and autonomic dysfunction
People living with chronic fatigue syndrome (ME/CFS) often show signs of autonomic nervous system imbalance, including reduced vagal tone. This shows up as difficulty recovering from exertion, poor sleep quality, and an immune system that seems stuck in overdrive. The vagus nerve normally helps shift your body from stress mode into recovery mode. When vagal function is impaired, your system struggles to downregulate after activity, creating a cycle where even minor exertion leads to prolonged exhaustion.
POTS, dysautonomia, and chronic pain conditions
Postural orthostatic tachycardia syndrome (POTS) and other forms of dysautonomia involve problems with how your autonomic nervous system regulates heart rate, blood pressure, and circulation. The vagus nerve plays a central role in cardiovascular regulation, and reduced vagal tone contributes to the racing heart and blood pressure fluctuations characteristic of these conditions. Fibromyalgia and other chronic pain conditions also show connections to vagal dysfunction, with research suggesting that impaired vagal activity contributes to central sensitization, where your nervous system becomes overly reactive to pain signals.
When to see a professional about vagus nerve issues
Self-care techniques like cold exposure, breathing exercises, and humming can genuinely improve vagal tone for many people. Sometimes, though, the nervous system needs more support than lifestyle changes alone can provide.
Red flags that need medical attention
Some symptoms suggest a structural or neurological issue with the vagus nerve itself, not just poor vagal tone. See a doctor if you experience fainting or near-fainting episodes, especially with changes in posture. Severe heart rate irregularities, such as your heart racing or dropping dramatically without clear cause, also warrant evaluation. Difficulty swallowing, chronic hoarseness, or a persistent feeling that food is stuck in your throat can indicate vagus nerve compression or damage. These concerns require diagnostic testing like autonomic function assessments or HRV monitoring.
When therapy is the right next step
Functional vagal tone, meaning how well your nervous system shifts between states, often responds well to therapeutic approaches. Consider professional therapy if you’re dealing with persistent anxiety or depression that doesn’t lift despite lifestyle changes. A history of trauma, chronic stress patterns you can’t seem to break, or feeling stuck in fight-or-flight mode are all signs that your nervous system might benefit from guided support.
Therapists trained in polyvagal approaches understand how trauma and chronic stress reshape nervous system responses. They can help you recognize your body’s patterns and build capacity for regulation that feels out of reach on your own.
If you’re experiencing persistent anxiety, depression, or difficulty recovering from stress, a licensed therapist can help you understand your nervous system patterns. ReachLink’s free assessment takes just a few minutes and connects you with a therapist at your own pace, with no pressure to commit before you’re ready.
Getting support for nervous system regulation
Your vagus nerve influences far more than most people realize, connecting your physical state to your emotional wellbeing in ways that explain why some symptoms resist conventional treatment. Understanding these patterns is the first step. Actually shifting them often requires guidance from someone who understands how trauma and chronic stress reshape nervous system responses.
If you’re experiencing persistent anxiety, difficulty calming down after stress, or feeling stuck in survival mode, working with a therapist trained in nervous system approaches can help. ReachLink’s free assessment takes just a few minutes and connects you with a licensed therapist who specializes in vagal regulation and trauma-informed care, with no pressure to commit before you’re ready.
FAQ
-
How can therapy help improve vagus nerve function and reduce anxiety?
Therapy approaches like cognitive behavioral therapy (CBT) and mindfulness-based interventions can help activate the vagus nerve through relaxation techniques, breathing exercises, and stress reduction strategies. These therapeutic methods teach you how to shift from a fight-or-flight state to a calm, regulated state, which naturally stimulates healthy vagus nerve function and reduces anxiety symptoms.
-
What therapeutic techniques are most effective for stress recovery and emotional regulation?
Several evidence-based approaches are particularly effective, including dialectical behavior therapy (DBT) for emotional regulation skills, somatic therapy for body awareness, and acceptance and commitment therapy (ACT) for stress management. Many therapists also incorporate breathing techniques, progressive muscle relaxation, and mindfulness practices that directly support vagus nerve activation and stress recovery.
-
When should someone consider therapy for chronic stress or anxiety symptoms?
Consider therapy when stress or anxiety interferes with daily functioning, relationships, work performance, or sleep patterns. If you experience persistent worry, physical tension, digestive issues, or difficulty recovering from stressful events, these may indicate that your nervous system needs support. Therapy can be beneficial even for mild symptoms as a preventive measure and to build resilience.
-
What can I expect during therapy sessions focused on stress and anxiety management?
Sessions typically include learning about the mind-body connection, practicing specific coping strategies, and developing personalized stress management techniques. Your therapist may teach breathing exercises, help you identify stress triggers, and work with you to develop healthy response patterns. Many approaches also include homework assignments to practice techniques between sessions.
-
How does telehealth therapy work for treating stress-related mental health concerns?
Telehealth therapy provides the same quality of care as in-person sessions, with the added convenience of accessing treatment from home. This can actually reduce stress for many people by eliminating travel time and creating a comfortable environment for therapy. Licensed therapists can effectively teach stress management techniques, breathing exercises, and coping strategies through video sessions, making mental health support more accessible.
